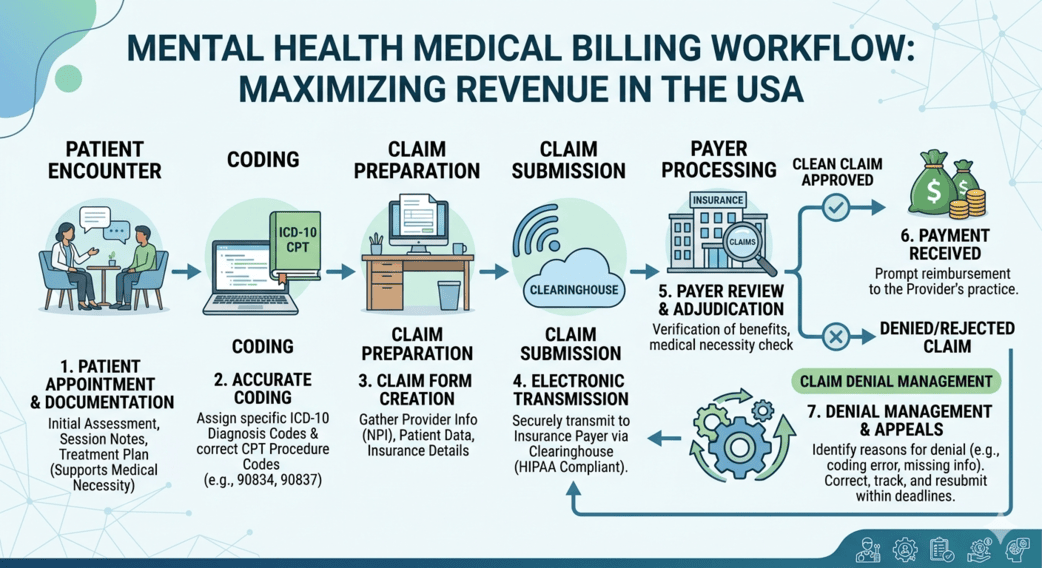
Mental health practices across the United States are experiencing a surge in demand. Therapists, psychologists, psychiatrists, and counseling centers are seeing more patients than ever before. While this growth is positive, it also brings complex administrative challenges. One of the biggest challenges providers face today is managing accurate billing and coding while maintaining compliance with constantly evolving healthcare regulations.
Mental health billing services play a crucial role in ensuring providers receive timely reimbursements while allowing them to focus on patient care. Unlike general medical billing, mental health billing involves unique coding structures, strict documentation requirements, and payer-specific policies that require specialized expertise.
Practices that rely on experienced professionals or specialized mental health billing specialist companies can reduce claim denials, improve revenue cycles, and maintain compliance with Medicare and private insurance requirements.
Key reasons mental health practices rely on professional billing support
• Accurate coding and documentation help prevent claim denials and payment delays
• Dedicated billing experts understand payer policies for behavioral health services
• Efficient claim submission improves cash flow and revenue cycle performance
• Compliance monitoring helps avoid legal and regulatory risks
• Providers gain more time to focus on patient care rather than administrative tasks
As mental health practices expand, many providers now choose outsourcing mental health billing and coding to experienced teams who understand the complexities of behavioral healthcare reimbursement.
Understanding Mental Health Billing and Why It Is Different
Mental health billing differs significantly from standard medical billing. Services such as psychotherapy, psychiatric evaluations, counseling sessions, and medication management have specialized CPT codes and documentation requirements.
Coding and billing for mental health services also require careful attention to treatment duration, therapy type, and patient diagnosis. Insurance companies often have strict policies regarding therapy session limits, authorization requirements, and reimbursement rules.
Medical billing for mental health therefore requires professionals who understand both clinical documentation and payer requirements. Even small mistakes in coding can lead to rejected claims or delayed payments.
Providers offering behavioral and mental health billing services often work with therapists, psychiatrists, group practices, rehabilitation centers, and community mental health clinics. Each of these settings requires different billing strategies and documentation standards.
For many clinics, working with a mental health billing company ensures that billing processes remain accurate and compliant while minimizing revenue leakage.
Key Components of Mental Health Billing Services
A comprehensive mental health billing services company typically manages several critical tasks within the revenue cycle. These services ensure smooth claim processing from patient registration to final reimbursement.
Patient eligibility verification is the first step in the process. Verifying insurance coverage ensures that billing for mental health services follows payer policies and prevents unexpected claim denials.
Coding accuracy is another essential element. Mental health billing professionals apply the correct CPT and ICD codes for therapy sessions, diagnostic evaluations, and psychiatric treatments.
Claim submission and management also play a central role. Billing specialists submit claims electronically, monitor their status, and follow up with insurers to ensure timely payments.
Denial management is equally important. Many billing companies for mental health analyze rejected claims, correct errors, and resubmit them to maximize reimbursements.
These services together form a complete mental health billing solution that helps practices maintain steady revenue streams while reducing administrative burdens.
Why Many Providers Choose Outsourcing Mental Health Billing
Administrative workload is one of the biggest challenges for mental health professionals. Therapists and psychiatrists often spend hours each week managing insurance paperwork and claim submissions.
Outsourcing mental health billing allows providers to delegate these tasks to experts who specialize in behavioral health reimbursement.
An outsourced billing team typically handles claim submissions, coding updates, denial management, and insurance follow-ups. This ensures that billing processes remain efficient and compliant with healthcare regulations.
Outsourced billing for mental health also provides scalability. As practices grow, billing requirements increase. Working with experienced mental health billing specialist companies allows providers to manage larger patient volumes without expanding internal administrative teams.
Many clinics also seek cost efficiency when choosing billing partners. Some providers search for a cheap outsource mental health billing company that can deliver professional services without increasing operational expenses. However, reliability, compliance, and industry expertise should always be the top priorities when selecting a billing partner.
Benefits of Working With Specialized Mental Health Billing Companies
Choosing a specialized mental health billing company offers several advantages compared to general billing providers.
A top mental health billing company understands the unique needs of behavioral healthcare practices. This includes knowledge of therapy codes, payer policies, telehealth billing guidelines, and documentation standards.
Experienced billing companies for mental health also maintain strong relationships with insurance payers, which helps resolve claim issues more quickly.
Another major benefit is improved revenue cycle performance. Accurate billing mental health processes reduce claim rejections and accelerate reimbursement timelines.
Mental health providers who partner with the best mental health billing services company often experience higher collection rates and fewer administrative headaches.
Specialized billing teams also stay updated with changing healthcare regulations, ensuring compliance with Medicare, Medicaid, and commercial insurance guidelines.
Mental Health Credentialing and Compliance
Credentialing is another essential aspect of successful billing for mental health providers. Insurance companies require practitioners to be properly credentialed before they can submit claims for reimbursement.
Mental health billing and credentialing services help therapists and psychiatrists complete provider enrollment, maintain updated credentials, and manage payer contracts.
Without proper credentialing, even correctly submitted claims can be rejected by insurance companies.
Credentialing experts ensure that providers meet payer requirements and maintain active participation in insurance networks. This allows clinics to expand their patient base while ensuring that billing for mental health therapists proceeds smoothly.
Credentialing services also help practices maintain regulatory compliance and avoid delays in reimbursement.
Medicare and Insurance Billing Challenges
Many mental health providers treat patients covered by Medicare or Medicaid. Billing medicare for mental health services requires strict adherence to federal guidelines and documentation standards.
Medicare typically covers services such as psychiatric evaluations, individual therapy, group therapy, and medication management. However, each service must be documented carefully and coded accurately.
Mental health medical billing professionals ensure that claims meet Medicare requirements and include all necessary documentation.
Private insurance companies also have their own policies regarding therapy sessions, treatment limits, and authorization requirements. A reliable mental health billing services provider helps practices navigate these policies while maintaining compliance.
Choosing the Best Mental Health Billing Services Company
Selecting the right billing partner is an important decision for any mental health practice. Providers should evaluate several factors before working with a mental health billing company.
Experience in behavioral healthcare billing is one of the most critical considerations. A provider specializing in behavioral & mental health billing services will understand therapy codes, payer requirements, and compliance regulations.
Technology infrastructure also plays an important role. Modern billing solutions should integrate with electronic health record systems and provide real-time reporting for practice managers.
Transparency and communication are equally important. Providers should receive clear reports about claims, reimbursements, and denial rates.
Clinics searching for the best mental health billing services often look for companies that offer customized solutions tailored to their practice size and specialty.
Many successful practices partner with the best mental health billing company that combines experienced staff, advanced billing systems, and comprehensive support.
The Future of Mental Health Billing Solutions
As the demand for mental health care continues to grow, billing systems are also evolving. Telehealth services, integrated healthcare models, and value-based reimbursement programs are transforming the way billing for mental health services operates.
Modern mental health billing solutions now include automated claim processing, advanced analytics, and improved payer communication systems.
These technologies help billing teams detect potential errors before claims are submitted, reducing denial rates and improving reimbursement timelines.
Outsourcing mental health billing has therefore become a strategic decision for many clinics seeking to improve efficiency and financial performance.
Reliable billing services for mental health clinics not only manage administrative tasks but also provide valuable insights that help practices grow sustainably.
Healthcare organizations that invest in professional billing services for mental health can focus more on delivering high-quality patient care while maintaining strong financial performance.
In the evolving healthcare landscape, specialized billing expertise is becoming an essential component of successful mental health practices.
Toward the end of the revenue cycle process, practices often benefit from working with experienced partners that provide comprehensive support including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. Organizations like 247 Medical Billing Services help healthcare providers streamline operations and improve financial outcomes while maintaining compliance with healthcare regulations.
Conclusion
Mental health practices face unique billing challenges that require specialized knowledge, accurate coding, and strict compliance with payer policies. Managing these processes internally can be time-consuming and often leads to claim denials or revenue loss.
Professional mental health billing services provide the expertise needed to streamline billing operations, improve claim acceptance rates, and ensure timely reimbursements. Whether a practice chooses in-house billing or outsourcing mental health billing, the goal remains the same: maintaining financial stability while delivering quality patient care.
With the right billing partner, mental health providers can focus on supporting patient wellbeing while their administrative and revenue cycle processes operate efficiently in the background.
Frequently Asked Questions
What are mental health billing services
Mental health billing services involve managing insurance claims, coding, claim submissions, and reimbursement processes for therapists, psychologists, psychiatrists, and mental health clinics.
Why do mental health providers outsource billing
Many providers choose outsourced billing for mental health to reduce administrative workload, improve claim accuracy, and ensure compliance with insurance policies.
How does mental health billing differ from regular medical billing
Mental health billing involves specialized therapy codes, session time documentation, and payer rules that differ from general medical procedures.
What services are included in mental health billing solutions
Comprehensive solutions typically include eligibility verification, coding, claim submission, denial management, payment posting, reporting, and credentialing support.
How can a mental health billing company improve revenue
An experienced billing team reduces claim denials, ensures correct coding, follows up on unpaid claims, and improves overall revenue cycle efficiency for mental health practices.